Our Approach
Approach
Approach
Peripheral CB1r Blockade
Our extensive knowledge of the CB1 receptor (CB1r) blockade propels our drug discovery and development efforts of next generation CB1 receptor blockers. The therapeutic relevance of the peripheral CB1 pathway is well understood and is implicated in the pathophysiology of a majority of metabolic and fibrotic diseases which pertains to the lungs, pancreas, liver, kidneys and GI tract. The mechanism of action of Inversago’s molecules seeks to address the safety limits associated with first generation, centrally acting CB1r blockers, allowing the company to exploit their full therapeutic potential.
Dr. George Kunos, a world expert in CB1 receptors from the NIH in the US, has extensively demonstrated that peripherally-acting CB1r blockade provides equivalent therapeutic potential compared with centrally-acting therapeutics in the treatment of metabolic and fibrotic conditions with an improved safety profile.
See also references 1 to 8 at bottom of the page.
Mechanism of Action of Peripheral CB1 Blockade
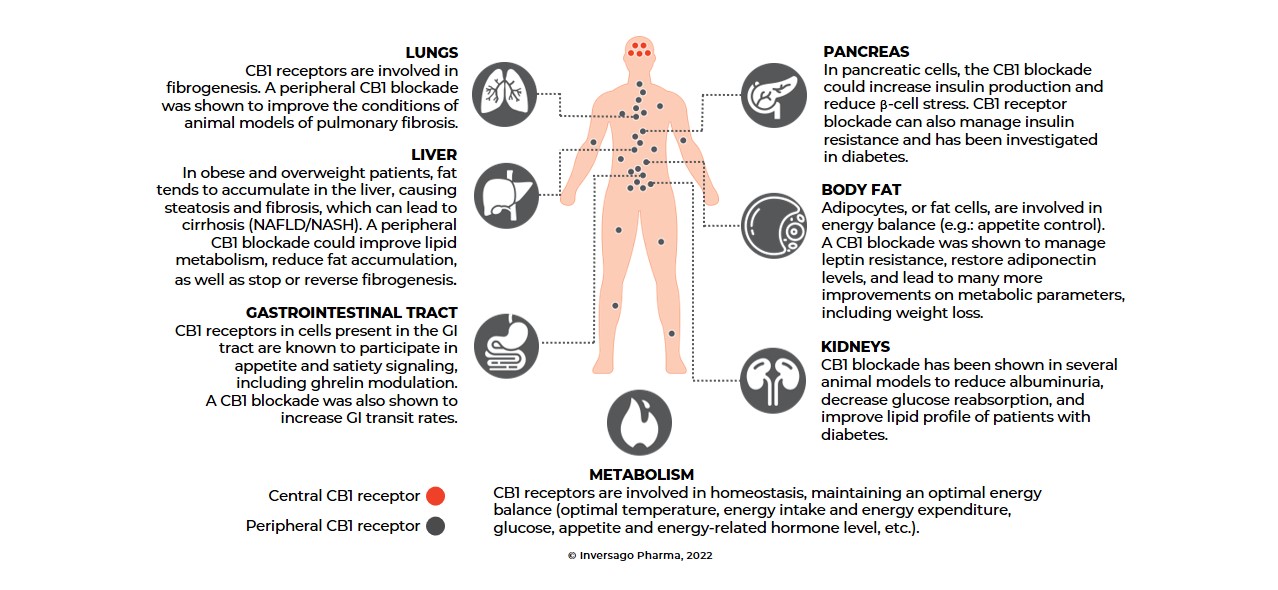
The Endocannabinoid System
CB1 Receptors: Signaling the Brain from the Periphery
The endocannabinoid system is responsible for both homeostasis and equilibrium of the human metabolism. It is involved in regulating several pathways linked to energy intake, reserves, and overall expenditure. To regulate these pathways, the CB1 receptor may be activated and deactivated, affecting many metabolic pathways involving several enzymes and proteins, such as leptin, insulin, and ghrelin.
The highest density of CB1 receptors is in the brain. However, diverse cell types outside of the central nervous system, including hepatocytes, β-cells, adipocytes, myocytes, and epithelial cells of the GI tract, also express the CB1 receptor.
The peripheral endocannabinoid system is now recognized as an important driver observed with first generation CB1 antagonists like rimonabant. As such, we believe next generation peripherally acting CB1 receptor blockers have the potential to control metabolic diseases better and more safely.
Metabolism, which refers to all life-sustaining processes occurring at a chemical level within living organisms, fulfills three purposes: converting food to energy to fuel cellular activity, using that energy to elaborate key components (proteins, lipids, nucleic acids, carbohydrates), and eliminating nitrogen (ammonia, urea, uric acid and creatinine).
In optimal conditions, metabolism functions in a state of balance, or homeostasis, regulating various parameters such as body temperature, energy intake and expenditure, glucose, appetite and energy-related levels, etc. The endocannabinoid system, via CB1 receptors, contributes to homeostasis by influencing appetite, lipid metabolism, glycemic control and the overall energy balance.
Any medical condition leading to a disruption in homeostasis, such as obesity, type 1 and type 2 diabetes or is considered a metabolic disorder. To address the pathophysiology of these indications, Inversago focuses its research and development on regulating the peripheral CB1 receptors, which are involved in many of these conditions.
References
1. Dao M et al. Cannabinoid Receptor 1 Inhibition in Chronic Kidney Disease: A New Therapeutic Toolbox. Front. Endocrinol., 07 July 2021 Sec. Cellular Endocrinology Volume 12 – 2021 doi.org/10.3389/fendo.2021.720734
2. Liu Z, Iyer MR, Godlewski G, et al. Functional Selectivity of a Biased Cannabinoid-1 Receptor (CB1R) Antagonist. ACS Pharmacol Transl Sci. Published online April 8, 2021. pubs.acs.org/doi/abs/10.1021/acsptsci.1c00048
3. Crater GD, Jourdan T, Jacquot L, Degrace P, Verges B. MO608: INV-202, A CB1 Receptor Blocker, Reduces Renal Injury in A Murine Model of Streptozotocin (STZ)-Induced Type-1 Diabetes. European Renal Association; 2022 May 18; Paris, France. c2022. academic.oup.com/ndt/article/37/Supplement_3/gfac076.001/6577705
4. Crater GD, Gaucher G, Harvey M, Ravenelle F. INV-101, a cannabinoid receptor-1 inverse agonist, reduces fibrosis in a bleomycin mouse model of IPF. European Respiratory Journal 60 (suppl 66) 171; DOI: 10.1183/13993003.congress-2022.171 Published 1 December 2022 erj.ersjournals.com/content/60/suppl_66/171
5. Bowles NP, Karatsoreos IN, Li X, et al. A peripheral endocannabinoid mechanism contributes to glucocorticoid-mediated metabolic syndrome. Proc Natl Acad Sci. 2015;112(1):285-290. dx.doi.org/10.1073/pnas.1421420112
6. Cinar R, Iyer MR, Kunos G. The therapeutic potential of second and third generation CB1R antagonists. Pharmacol Ther. 2020;208:1-24. doi.org/10.1016/j.pharmthera.2020.107477
7. Cinar R, Gochuico BR, Iyer MR, et al. Cannabinoid CB1 receptor overactivity contributes to the pathogenesis of idiopathic pulmonary fibrosis. JCI Insight. 2017;2(8):e92281. doi.org/10.1172/jci.insight.92281
8. Cinar R, Iyer MR, Liu Z, et al. Hybrid inhibitor of peripheral cannabinoid-1 receptors and inducible nitric oxide synthase mitigates liver fibrosis. JCI Insight. 2016;1(11):e87336. dx.doi.org/10.1172/jci.insight.87336


